Right After Surgery
4th of January 2021
I woke up in the surgery room and went into the ICU. The first assessment was by a neurologist making basic tests; one key was my legs. They were all good.
What happened right after that was that I met my wife, so I could be given CBD (this was arranged by the Neurosurgeon before this). I was also given and approved of the Bromelain that I had and took as per the protocol that Michelle Gerencser set. I committed to Bromelain for a week.
The next morning, I was given different medications to ensure the pain was minimal.
In the morning, all the tests showed that I was doing well, and they walked me to my room at 11 AM (earlier than usual for other patients, as they said I was doing better)
First 5 Days (at hospital)
4th–9th of January 2020
Below are the medications that I was given by the doctors in the hospital:
|
Day from surgery |
Pain killers |
Enoxaparin 5 days |
Omeprazol 15 days |
Dexamethasona 15 days |
|
1st day |
Took it |
Took it |
Took it |
Took it |
|
2nd day |
I replaced one for another |
Took it |
Took it |
Took it |
|
3rd day |
Stopped second type |
Asked to stop |
Took it |
Took it |
|
4th day |
only Paracetamol and Ibuprofen |
Asked to stop |
Took it |
Took it |
|
5th day |
same as below |
Asked to stop |
Took it |
Took it |
|
Notes |
I’m hallucination because of |
I arranged it with the doctor too. |
Stopped it on the 6th day after |
Stopped in 10 days instead of 15, |
I asked the doctor whether I had any antibiotics, and they said that I had them for three days only.
The below shows the symptoms I was suffering while I was in the hospital:
|
Day from surgery |
Headache |
Comprehension What’s Heard (higher means better) |
Reading/ Writing |
Hallucination (higher means worse) |
Sleeping |
|
1st day |
1 to 3 |
1 |
1 |
9 |
6 |
|
2nd day |
1 to 3 |
1 |
1 |
9 |
5 |
|
3rd day |
1 to 9 |
2 |
1 |
8 |
2 + 2 |
|
4th day |
1 to 9 |
3 |
1 |
8 |
3 |
|
5th day |
1 to 9 |
3 |
1 |
8 |
4 |
|
Notes |
More than half the time, headache are around 6 |
I walked out poorly after leaving |
I could read the mobile, read e-mails or respond |
Mostly weird characters that move “away” from me. |
They do not have melatonin in the hospital |
On the third day, the doctor was surprised, and he said that I am ready to leave on the third day and that I can remove what’s on my brain. However, he felt that it’d be better to stay at the hospital until the five days were over.
The images below are from a few minutes before it was removed
Pathology is Out!
9th of Jan 2021
Dr. Oliver: Future Options
When we spoke about Practice for Human Genetics Tübingen, spent time reviewing what they do. He told me that the concepts exist in Spain, but what they are doing is more advanced. His recommendation was that going for chemo is best taken with Dr. Saskia Biskup.
3 Weeks Post-Hospital
From the 9th of January 2021 onwards
After leaving the hospital, I stayed in Spain for 9 days and then left for Amman, Jordan. Before leaving for Spain, the doctor informed me it would be best to do a CT Brain to ensure I’m safe (and that took place, and I was safe to travel).
Pain Control and Sleep
Diet
Symptoms Remaining
|
After leaving |
Comprehension |
Reading/ (higher |
Hallucination (higher means better sleep) |
|
1st |
4 |
2 |
5 |
|
2nd |
5 |
3 |
4 |
|
3rd |
5 |
4 |
3 |
|
Notes |
Way worse than before surgery |
Way worse than before surgery |
It is improving |
Seizure Control
EEG
Vision Issues After Brain Surgery
These include how the five days in the hospital were, what I suffered from, and what I was doing well.
Most importantly, the Pathology was out and I’m sharing here
Clearly, given that my left temporal lobe surgery is on the left, this means that possibly the right side is going to be affected.
The image on the right side explains how the area that will be touched during the surgery will be touched.
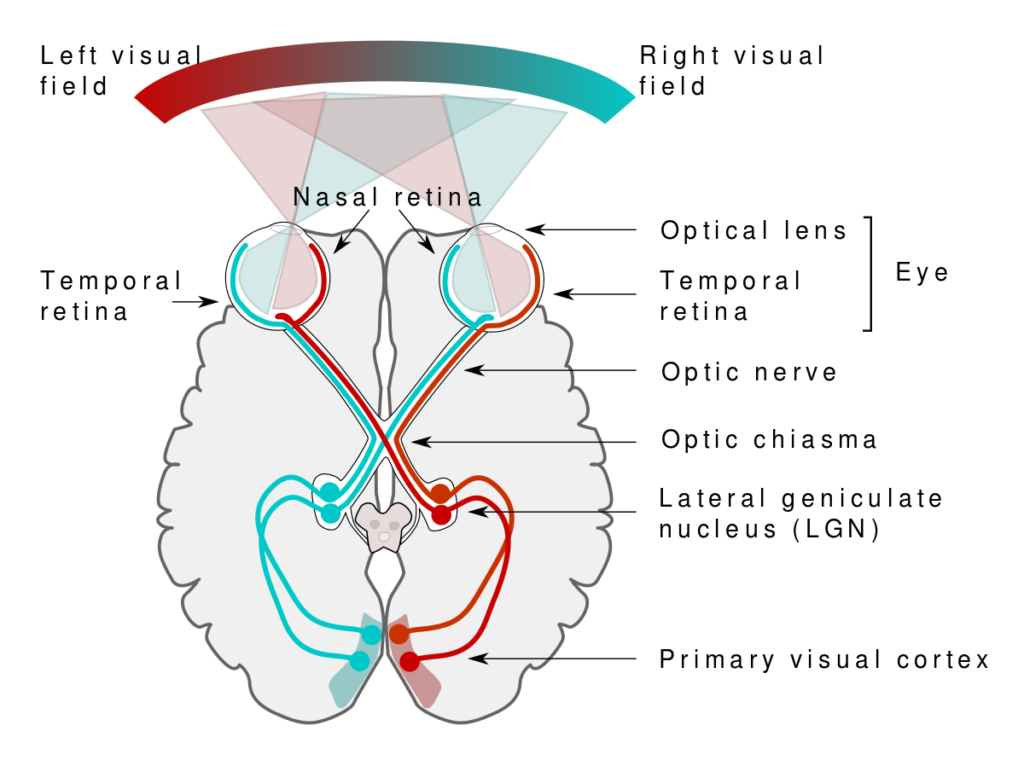
That’s what the doctor explained to me before the surgery, and he explained I may not be able to see things that are right far away from my right side, and accordingly, with time, I will be starting to physically see what I want to see.
The doctor was in fact surprised that I was seeing things clearly on the right before the surgery, given that the tumor is significant on the left side.
After surgery, a basic test by the doctor showed me clearly that I did lose my ability to see the “far away” right side without moving my head.
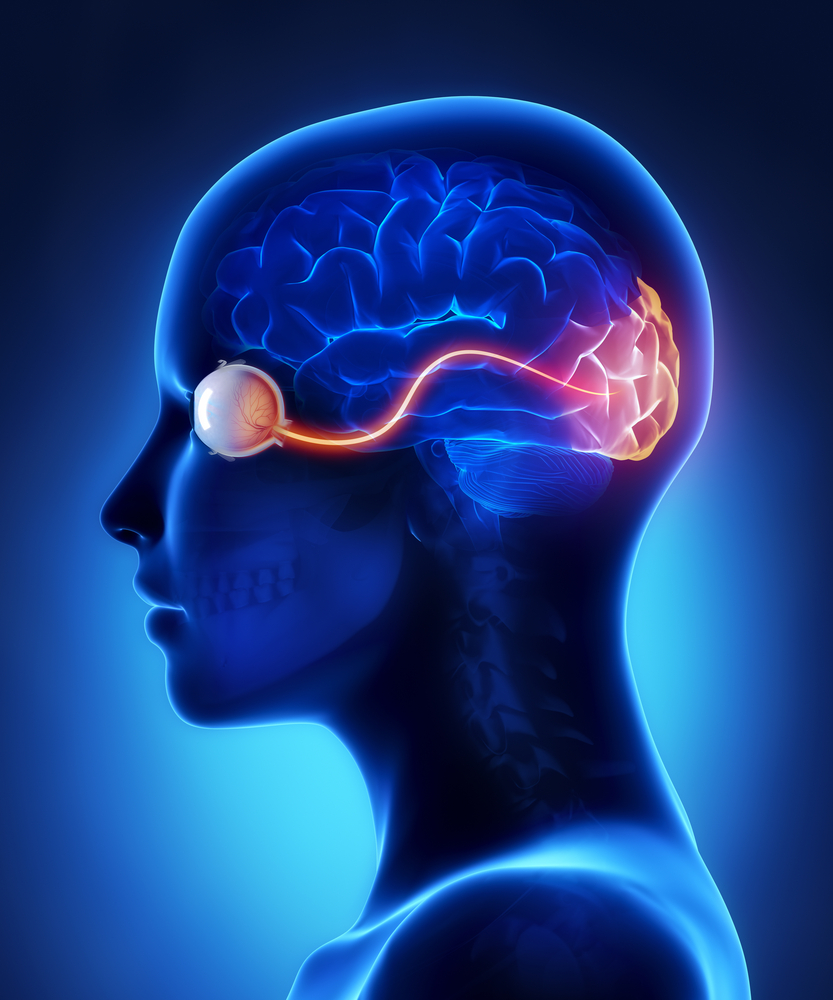
Double Visions
In the first week, I used to see most of what I read shown doubled next to each other. With time, that has become far less, but it is still happening (3 weeks later). However, if I look at the right side, I still see the double visions for the first 1 to 2 seconds, and then they improve.
Supplements During the 3 Weeks
|
After leaving |
1st |
2nd |
3rd |
|
Vitamin D |
Y |
Y |
Y |
|
Resvero |
N |
Y |
Y |
|
Turmero |
Y |
Y |
Y |
|
EnzymixPro |
Y |
Y |
Y |
|
Brain-E DHA |
N |
Y |
Y |
|
BDNF |
N |
N |
Y |
|
Complete E |
N |
Y |
Y |
|
EnteroVite |
Y |
Y |
Y |
All the things that I did not take on the first week of walking to the hospital were because I did not have them with me while I was in Spain.
Did Pathology Arrive Safely?
As planned weeks before travel, we had communicated with the hospital in Spain and we planned to execute right after surgery. The outcome was as follows:
Tumor Diagnostic: By Saskia Biskup, MD
I will be waiting for the outcome in 4 to 6 weeks to see the results!
Nagourney Cancer Institute: By Robert Nagourney, MD
The hospital did a great job preparing it during the surgery in order to send it to the United States. Sadly, the 4th of January until the 7th of January were not good days for them to deliver to the United States. At least four different shippers said that it can be delivered in 5 days, and in reality, that is too long (it won’t arrive in good shape)
Therefore, we lost the opportunity with Nagourney Cancer Institute, and they were informed.
NEXT: Second Month with Surprise
Click here to see how the second month went with difficulty
Click here to see how the second month went with difficulty
